Rumination disorder treatment for adults primarily focuses on Diaphragmatic Breathing techniques, also known as behavioral retraining. Unlike acid reflux treatments, this specialized breathing method relaxes the diaphragm and tightens the lower esophageal sphincter after eating. This prevents the increase in intra-abdominal pressure that triggers regurgitation, effectively retraining the body’s automatic digestive response.
What is Rumination Disorder in Adults?
Rumination disorder is a functional gastrointestinal condition characterized by the repetitive, effortless regurgitation of recently ingested food into the mouth. Unlike vomiting, which is forceful and often accompanied by nausea, rumination is often described as a reflexive action where food is brought back up, re-chewed, re-swallowed, or spat out. For many adults, this condition is chronic, misunderstood, and frequently misdiagnosed, leading to years of unnecessary medical interventions.
In the context of the New Zealand healthcare system, we are seeing an increasing awareness of this condition, particularly distinguishing it from standard eating disorders like Bulimia Nervosa or physiological issues like Gastroparesis. While it is classified under Feeding and Eating Disorders in the DSM-5, the underlying mechanism in adults is often an acquired behavioral habit involving the involuntary contraction of the abdominal wall muscles. This contraction increases gastric pressure, forcing the stomach contents upward against a relaxed lower esophageal sphincter.
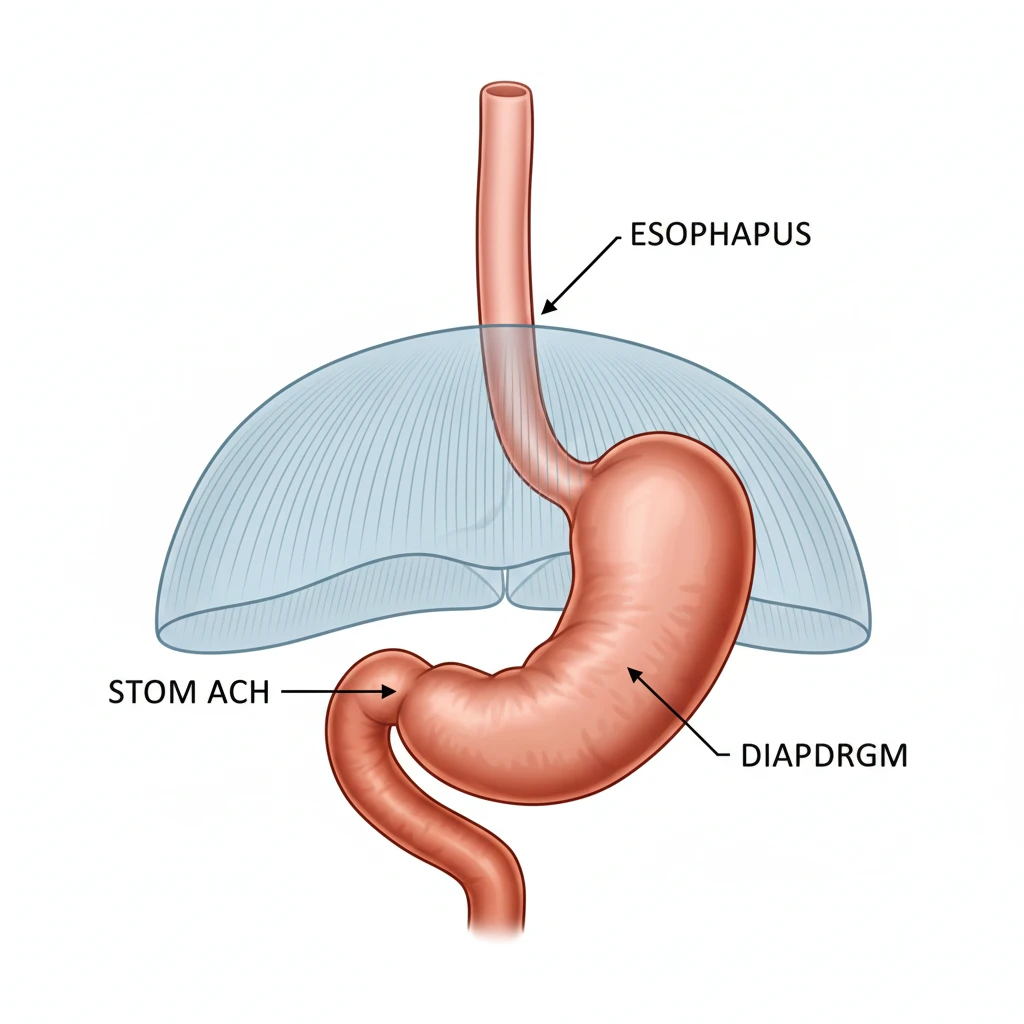
How to Distinguish Rumination from Reflux (GERD)?
One of the most critical steps in securing effective rumination disorder treatment for adults is accurately distinguishing the condition from Gastroesophageal Reflux Disease (GERD). In New Zealand primary care settings, patients often present with “reflux” symptoms and are prescribed proton pump inhibitors (PPIs) such as Omeprazole. However, for rumination disorder, these medications are largely ineffective because the mechanism is behavioral, not acid-related.
Key Differences in Symptoms
The distinction lies in the timing and the nature of the regurgitated material:
- Taste and Texture: In rumination disorder, the food comes up undigested and often tastes similar to how it did when swallowed. It is generally not acidic or bitter. In contrast, GERD involves acidic, partially digested liquid that causes a burning sensation (heartburn).
- Timing: Rumination typically occurs within 15 to 30 minutes of starting a meal. It happens while eating or immediately after. GERD episodes can happen hours later, often when lying down or sleeping at night.
- Effort and Nausea: Rumination is effortless and rarely accompanied by nausea or retching. It is a distinct physical sensation of food reversing course. Vomiting or severe reflux often involves significant physical distress and nausea.
- Response to Medication: If you have been adhering to a high dose of acid-suppression medication prescribed by your GP without any reduction in regurgitation volume, this is a strong clinical indicator of rumination disorder rather than refractory GERD.
Understanding these nuances is vital. Misdiagnosis leads to frustration and potential side effects from unnecessary long-term medication use. If your symptoms align more with the effortless regurgitation of fresh food, it is essential to discuss this specifically with your healthcare provider.
Behavioral Breathing Techniques for Recovery
The cornerstone of rumination disorder treatment for adults is diaphragmatic breathing. This is not merely a relaxation exercise; it is a physiological intervention designed to mechanically prevent the regurgitation reflex. When performed correctly, this technique increases the pressure at the esophagogastric junction, effectively creating a barrier that stops food from traveling upward.

The Diaphragmatic Breathing Protocol
To effectively treat rumination, this breathing technique must be applied specifically during and immediately after meals. The goal is to disengage the abdominal muscles from contracting and instead engage the diaphragm.
- Positioning: Sit comfortably with a straight spine. Place one hand on your upper chest and the other on your abdomen, just above your belly button.
- The Inhale: Inhale slowly and deeply through your nose. Focus on expanding your abdomen outward against your hand. Your chest should remain relatively still. This ensures the diaphragm is descending.
- The Exhale: Exhale slowly through pursed lips (as if blowing out a candle). Allow the abdomen to fall naturally.
- Timing is Critical: This breathing pattern should be initiated at the very start of a meal. If you feel the urge to regurgitate, stop eating, put down your utensils, and focus entirely on the breathing until the urge passes.
- Post-Prandial Practice: Continue this breathing for 10 to 15 minutes after finishing your meal, as this is a high-risk window for regurgitation.
Many patients in New Zealand find success by working with a physiotherapist or a specialized Speech-Language Therapist (SLT) to master this technique. It requires consistency; the brain must “unlearn” the habit of tightening the abs after swallowing.
Impact on Social Eating and Nutrition
Beyond the physical symptoms, rumination disorder can have a profound impact on an adult’s quality of life, particularly regarding social interactions and nutritional health. In a culture like New Zealand’s, where social bonding frequently occurs over food—be it a BBQ, a café brunch, or a family dinner—the fear of regurgitation can lead to isolation.
Social Isolation and Anxiety
Adults with untreated rumination disorder often develop compensatory behaviors to hide their condition. They may avoid eating in public entirely, chew excessively to reduce the volume of food, or excuse themselves to the bathroom frequently during meals. This vigilance creates a cycle of anxiety. Anxiety, in turn, can exacerbate the abdominal tension that triggers rumination, creating a self-perpetuating loop. Addressing the mental health aspect is often a necessary component of rumination disorder treatment for adults.

Nutritional and Physical Consequences
While some adults maintain a healthy weight, many suffer from unintentional weight loss and malnutrition because a significant portion of their caloric intake is regurgitated and expelled. Furthermore, even though the regurgitant is not as acidic as classic reflux, repeated exposure can still damage dental enamel over time. Electrolyte imbalances are also a risk if the volume of loss is high. Recovery involves working with a Dietitian to ensure that as the behavioral therapy takes effect, nutritional density is restored.
Specialist Speech Language Therapists in NZ
Finding the right care provider is the final piece of the puzzle. In New Zealand, the pathway to diagnosis and treatment often begins with a General Practitioner (GP) but should ideally lead to a specialist familiar with functional gastrointestinal disorders.
The Role of Speech-Language Therapists (SLTs)
While it may seem counterintuitive, Speech-Language Therapists are often the primary providers for rumination disorder treatment for adults. SLTs specialize in the mechanics of swallowing and the upper digestive tract. In NZ, there are SLTs specifically trained in behavioral interventions for upper GI disorders.
When seeking a referral, ask your GP or Gastroenterologist about SLTs who specialize in “esophageal disorders” or “functional GI disorders.” These specialists can use biofeedback—a technique where you watch a visual display of your muscle activity—to help you learn how to relax the abdominal muscles effectively during eating.
Navigating the System: Public vs. Private
Te Whatu Ora (Public System): Access to specialized SLTs for rumination disorder through the public hospital system is possible but may require a referral from a Gastroenterologist. Wait times can vary significantly by region.
Private Practice: There are private Speech-Language Therapy clinics in major centers like Auckland, Wellington, and Christchurch that offer specific programs for rumination and laryngeal issues. Going private often allows for faster access and more intensive follow-up, which is crucial in the early stages of behavioral retraining.

Additionally, because of the behavioral nature of the condition, some patients benefit from the support of a Health Psychologist. They can assist with the anxiety surrounding eating and help reinforce the habit-reversal techniques taught by the SLT.
People Also Ask
Is rumination disorder considered an eating disorder?
Yes, Rumination Disorder is classified under “Feeding and Eating Disorders” in the DSM-5. However, unlike Anorexia or Bulimia, it is not typically driven by body image distortion or a desire to lose weight, but rather by an unconscious physical reflex.
Can rumination disorder be cured in adults?
Yes, the prognosis for adults is generally very good. With consistent application of diaphragmatic breathing techniques and behavioral retraining, the majority of patients see a significant reduction or total cessation of symptoms.
What medications treat rumination disorder?
There are no specific medications approved to cure rumination disorder. While Baclofen (a muscle relaxer) is occasionally used in refractory cases to relax the lower esophageal sphincter, the primary and most effective treatment is behavioral breathing therapy, not medication.
Does anxiety cause rumination disorder?
While anxiety does not directly cause the disorder, it is a significant exacerbating factor. Stress and anxiety can increase abdominal muscle tension, which makes the regurgitation reflex more likely to occur. Treating underlying anxiety often helps improve physical symptoms.
How is rumination disorder diagnosed?
Diagnosis is primarily clinical, based on the history of effortless regurgitation soon after eating. Doctors may use High-Resolution Esophageal Manometry to observe the pressure changes in the abdomen and esophagus to confirm the diagnosis and rule out other conditions.
Is rumination disorder rare in adults?
It is likely more common than statistics suggest due to high rates of misdiagnosis as GERD or refractory vomiting. As awareness grows among gastroenterologists and primary care physicians, more adults are being correctly identified and treated.